Katherine health researcher Alice Mitchell has dedicated much of her life to working with children dying from a completely preventable, life-threatening disease.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
But her work, along with a documentary she worked on, is turning that around.
With a background in midwifery, applied linguistics and medical anthropology, Dr Mitchell is passionate about eradicating rheumatic heart disease.
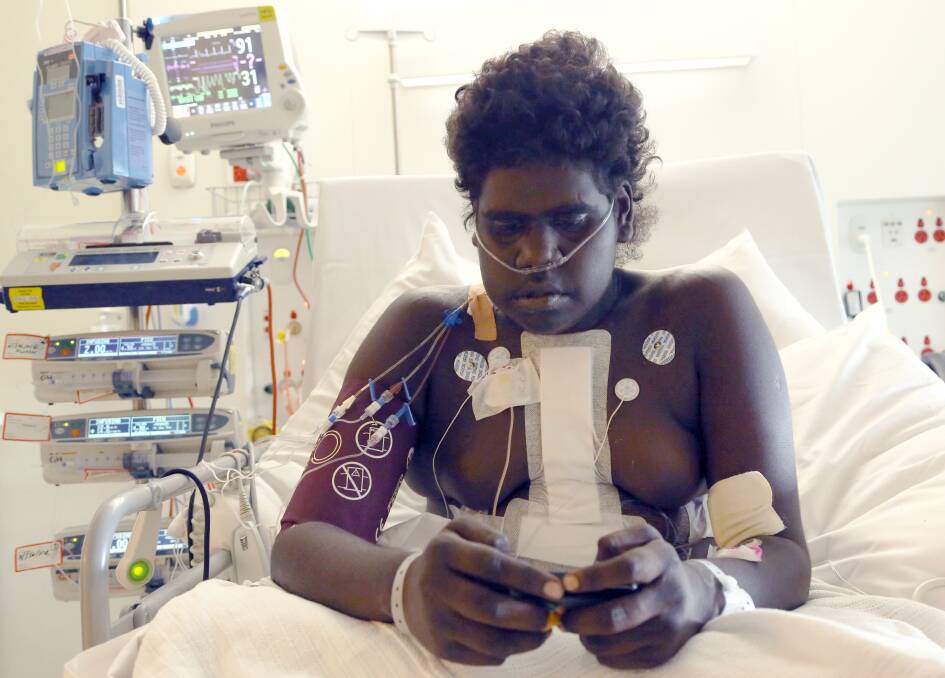
Confronted with countless cases of young children having their chests cut open, she is dedicated to the fight against one of the leading causes of death among young Indigenous people in remote communities.
In addition to creating a smartphone app helping those with the disease to keep on top of their treatment, she worked on Take Heart, a documentary released in 2016, which is gaining traction and getting people to take notice.

"This completely preventable disease is a shame for our country," Dr Mitchell said.
"If one child died in Melbourne there would be an outcry, but in these remote communities we have the highest rates in the world of a completely preventable disease and people down south don't know about it.
"The general public is not aware of it because they are so far removed."
In Katherine there are children walking around and going to school with the disease, and most of them won't make it past 30 years of age.
Dr Mitchell was working in the Katherine area as a remote nurse, diagnosing the disease in too many children (it threatens the lives of two per cent of all Indigenous Australians), when she was approached to help with the documentary.
"I met up with the producer and he wanted to film children with rheumatic heart disease and I was already working with these children.
"I had been working in the region in Katherine for a while so I knew how to engage with them appropriately and culturally.
"The producer of Take Heart (Mike Hill) is a really passionate and dynamic guy, he makes films for people who don't have a voice, and that takes courage.
"He told me that when he was first informed of this huge silent problem happening in the same country he was living in, he couldn't not make a film about it."
Dr Mitchell said her role in the film was mainly to assist Mike Hill in engaging with the interviewees in a culturally appropriate way.
Having spent a lot of time in remote communities working with patients, she had the knowledge and the trust.
"As he was interviewing kids I would be sitting on the sideline, and I would jump in if I saw something was about to be inappropriate," she said.
"We have two really different cultures interacting, and I had learnt the rules.
"In a way, the whole experience was fun. The kids we were working with were great, as were their families. And I believed in what we were making the film for."
Take Heart: The Quest to Rid Australasia of Rheumatic Heart Disease, released about two years ago, is now starting to gain traction.
The film has been used in Canberra to lobby the government to take action.
And two Katherine schools, MacFarlane Primary and Clyde Fenton Primary, have picked it up to ensure teachers are informed with the right information to make life-saving decisions.
But the film as a standalone is not enough to eliminate the disease.
Dr Mitchell said it will take a multi-pronged approach to get to the point of places like Cuba and the French Caribbean, who have seen dramatic falls in RHD, without the help of a vaccination.
"Nothing will improve unless housing improves," Dr Mitchell said.
"Going down that path we need to not just spend money, the houses have to be the right design and there needs to be maintenance.
"When you have dense living, which is actually a social strength in Indigenous society, infection spreads much faster.
"It starts with the strep germ, and if the shower doesn't work because the plumber can't get a flight from Darwin, or you can't wash your towel because there is no washing machine, you can see how infection can spread quite easily. It is a vicious cycle."
People working in the field have found there are significant issues with language barriers making it hard to communicate the importance of keeping on top of the life-saving treatment, often an injection of penicillin every 21 to 28 days.
"We are working to support community leaders who have had that 'penny drop' moment and will be able to make changes within the community," Dr Mitchell said.
"Because they speak the language they know the best way to connect and convey the appropriate information."

While scientists are working on a vaccine, 2018 Northern Territory Australian of the Year and the Territory's only paediatric cardiologist, Dr Bo Reményi, says we cannot wait.
"We need to take action now to prevent, identify and manage RHD - we cannot wait for a vaccine or other solutions because while we wait thousands of people will become ill, and hundreds will die."
Speaking at the 15th National Rural Health Conference, in March, Dr Reményi called for major political parties to commit to immediate community-led on the ground action to prevent and eliminate RHD.
"RHD is the best marker for disadvantage between Indigenous and non-Indigenous Australians," Dr Reményi said.
"Some of our communities have the highest rates in the world of this disease - young children are being subjected to painful treatment and even open heart surgery, and they are dying way too early.
"RHD is the greatest cause of cardiovascular inequality for Aboriginal and Torres Strait Islander people in this country. If we don't close the gap on RHD, we cannot close the gap between Indigenous and Non-Indigenous life and health outcomes."
While you're with us, you can now receive updates straight to your inbox each Friday at 6am from the Katherine Times. To make sure you're up to date with all the news, sign up here.

