Infection and antibiotic prescription rates among Indigenous children in the Katherine area are dangerously high.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
That's the finding of a study released yesterday by the Menzies Institute and Katherine's Sunrise Health Service examining antibiotic prescription rates in remote communities.
"Australian Aboriginal children in remote communities had exceptionally high levels of antibiotic prescriptions in comparison to Australian values," the report said.
"The high rates of antibiotic prescription are attributable to an underlying burden of disease that is substantially higher in Aboriginal children than non-Aboriginal children," it said.
Analysis of 124 children's health records from the Katherine East region found nine in ten had received antibiotics in their first year of life.
It also suggests Indigenous kids are receiving 12 prescriptions in their first two years, most commonly for inner-ear infections which often lead to hearing loss.
Data from the Pharmaceutical Benefits Scheme meanwhile suggests just half of Australians receive antibiotics at least once across their first four years.
As the study showed doctors were prescribing appropriately, researchers believe their findings demonstrate "the urgent need" to address the health gap between Indigenous and non-Indigenous Australians from birth.
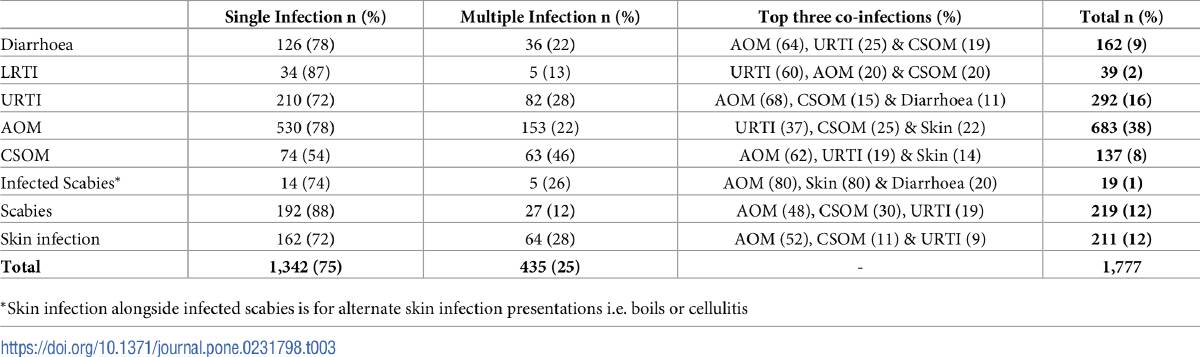
Acute inner ear (AOM), upper respiratory tract (URTI) and skin infections including infected scabies all frequently required prescription from remote healthcare professionals.
More reading:
"Treatment for otitis media alone accounted for 30 per cent of prescriptions," Lead Author Timothy Howarth said.
Otitis media (any inner ear infection) is endemic in Indigenous communities with up to nine in ten Indigenous children experiencing such infections at some point.
Their high prevalence has been linked to issues from family dysfunction to school attendance due to permanent damage to their hearing.
Scabies and other skin issues have also been shown to have severe social impacts beyond their physical symptoms for Indigenous kids.
Besides the rates of dangerous disease, high antibiotic prescription in itself is also concerning to researchers.
"Antibiotic use in infancy is associated with a long-term shift in the gut which may further increase the risk of chronic disease in this vulnerable population," the report said.
"High prescription rates in infancy may have some contribution to chronic disease later in life," it said.
While highlighting this and other health challenges still facing Indigenous children, Mr Howarth says the study does demonstrate strong responsibility from health professionals in prescribing the antibiotics.
"Even though the rate of prescriptions is higher we also found that the tracking of prescriptions here is significantly better than the wider Australian community," he said.
"Legislative requirements placed on nurses and Aboriginal Health Practitioners to supply and administer antibiotics was effective in limiting inappropriate antibiotic use in this setting," Dr Kearns said.
While you're with us, you can now receive updates straight to your inbox each Friday at 6am from the Katherine Times. To make sure you're up to date with all the news, sign up here.

